What Is It?
Total Hip Replacement is a surgical procedure we perform in Waterloo, Independence and Vinton. This surgery is meant to replace damaged portions of the hip joint with higher functioning, prosthetic components.
Total Hip Replacement is a surgical procedure we perform in Waterloo, Independence and Vinton. This surgery is meant to replace damaged portions of the hip joint with higher functioning, prosthetic components.
Much like the shoulder, the hip operates as a ball-and-socket joint and is one of your body’s largest joints. The hip joint forms at the meeting place of your femur and pelvis, and encourages a wide variety of leg movements. A doorknob-like head to the femur fits inside a socket within the pelvis, known as your acetabulum. Both the end of your femur and the inside of your acetabulum are covered with smooth cartilage, which cushions the bones and enables mobility. Various ligaments strengthen and hold the joint together, while a thin cover-layer of tissue releases small amounts of moisturizing fluid to further eliminate friction.
Arthritis is one of the most common causes of hip pain that requires surgical treatment.
Osteoarthritis is age-related, primarily affecting individuals 50 years of age or older. Over time, protective, mobilizing cartilage wears away, causing bones to painfully rub against each other.
Rheumatoid arthritis is an inflammatory disease that causes the moisturizing tissue to swell and thicken. Over time, this inflammation disrupts cartilage and stiffens movement in the hip joint.
Post-traumatic arthritis follows many serious hip and upper leg injuries. When ligaments and bones are damaged near the joint, cartilage can follow suit and become completely destroyed over time, even following the surgical treatment of major hip injuries. Severe fractures or dislocations of the joint may limit blood flow to the connected portion of the femur. This lack of blood flow may cause the bone’s surface to collapse and lead to arthritis.
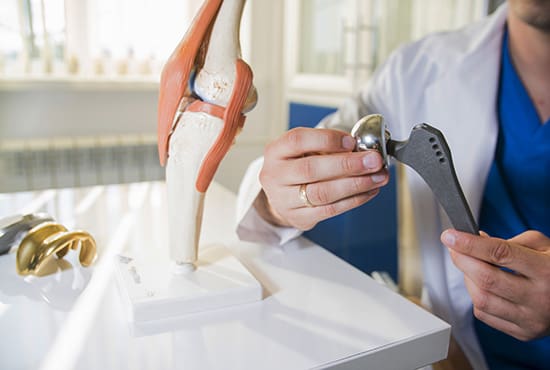
The overall goal of total hip replacement is to remove the portions of damaged bone and cartilage and replace them with higher functioning, prosthetic components. The femur’s doorknob-like head is removed and replaced by a metal or ceramic ball. This metal ball is attached to a long stem inserted into the femur. Damaged cartilage is removed within the socket and replaced by a fabricated metal socket, and press fit in place with special instruments. To complete the procedure, a plastic spacer is inserted between these newly fabricated body parts to provide a smoother operating surface for each component.
Prior to hip replacement surgery, your orthopedic surgeon will conduct a complete orthopedic evaluation consisting of X-rays, physical examinations, and a full inquiry into your medical history. Most patients who undergo hip replacement surgery are 50 years of age or older. Unfortunately, there are weight restrictions for your protection. If your BMI is greater than 35, you are at a greater risk of developing complications such as infection, blood clots, or much worse, not to mention, the components implanted will wear out at a faster rate, resulting in possibly more complications and even revision surgery. Therefore, you may be asked to lose weight prior to the procedure to reduce stress on your newly reconstructed hip, and reduce the risk of more major, possibly life threatening complications.
You may be asked to donate and store your own blood in the event that you need blood following surgery.
Arguably the most important way to prepare for your surgery is to plan and adjust your home situation as much as possible before-hand. Adjust movement expectations and allow yourself to recover in a rehabilitation-friendly environment. Fasten safety bars to your shower and along stairways, utilize firm pillows and chairs, and set up a fully functional recovery station where you’ll spend a majority of your recovery time.
Following the procedure, you’ll need to stay in the hospital overnight. Our medical team will closely monitor your newly reconstructed joint and wound and look to effectively manage your pain. You will begin a physical therapy program to rebuild strength and range of motion about the joint immediately. Physical therapy begins with standing and supported walking, but extends to more intense stretches and exercises as rehabilitation improves.
Upon leaving the hospital, the first few weeks of home care are vital to full rehabilitation. Maintaining your water-tight sterile and antimicrobial dressing, eating a balanced diet, and closely following your designated activity program are all ways to help ensure that your recovery process is positive in nature. Most patients are able to resume light, everyday activities within 3 to 6 weeks following surgery, but are unlikely to recover in full until at least 6 months after their procedure.